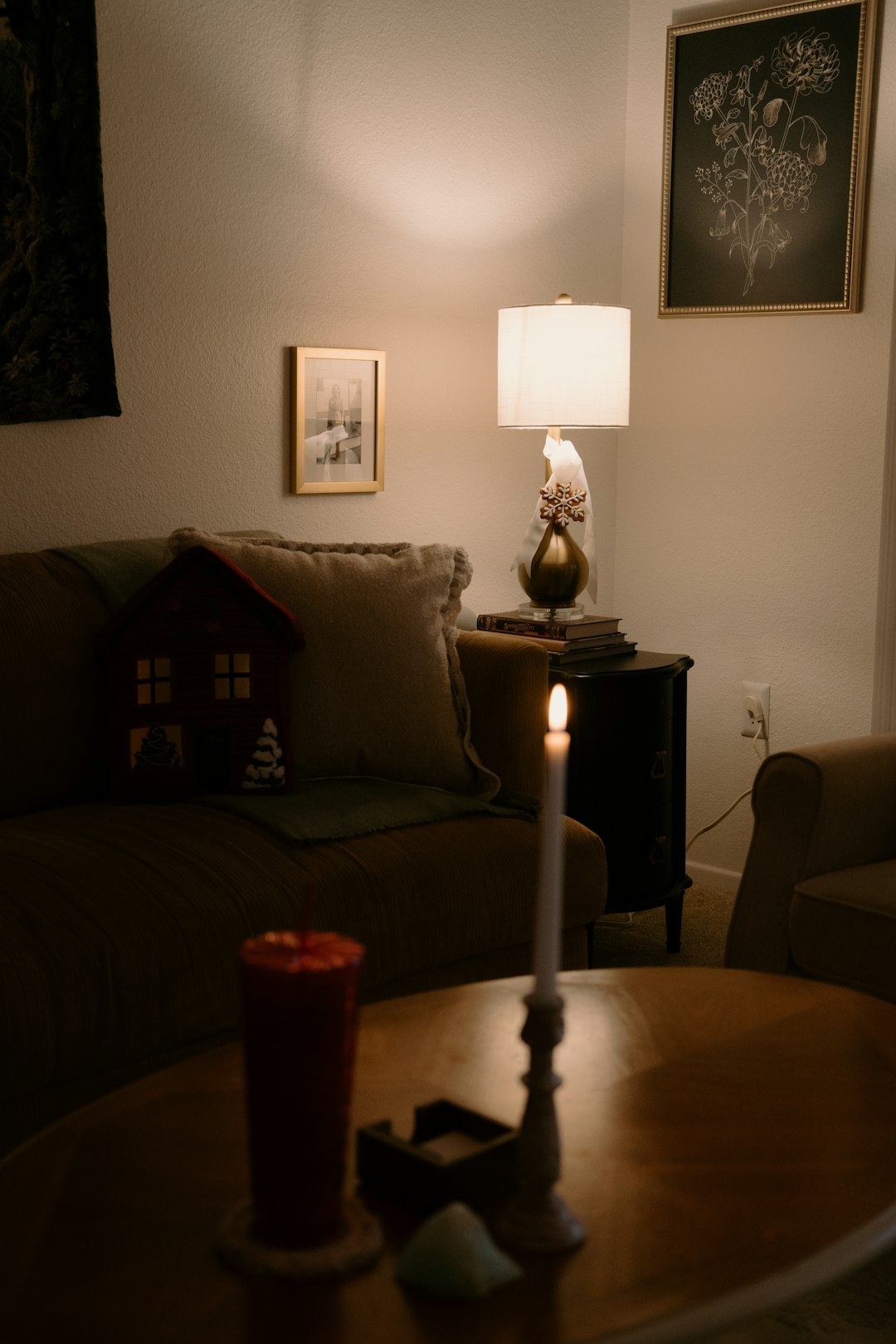
Home is more than a place. It is where memories live. It is where favorite chairs sit. It smells familiar. It feels safe. When someone is living with a serious illness, that comfort matters more than ever. This is where palliative care at home can make a big difference. It helps people feel better, stay comfortable, and enjoy life in ways that truly matter.
TLDR: Palliative care at home focuses on comfort, dignity, and quality of life for people with serious illness. It helps manage pain, stress, and symptoms while allowing patients to stay in familiar surroundings. Families also receive emotional and practical support. The goal is simple: more comfort, more meaning, and more good days at home.
Palliative care is often misunderstood. Some think it is the same as hospice. Others think it means giving up. That is not true. Palliative care is about support. It can happen at any stage of illness. It can be given alongside treatments like chemotherapy or dialysis. It is about living as well as possible, for as long as possible.
What Is Palliative Care at Home?
Think of it as a comfort team that comes to you. Doctors. Nurses. Social workers. Chaplains. Sometimes therapists. They work together. Their goal is to manage symptoms and reduce stress.
They help with:
- Pain control
- Shortness of breath
- Nausea and appetite problems
- Fatigue
- Anxiety and depression
- Sleep issues
But they do more than treat physical symptoms. They also support emotional and spiritual needs. They talk about fears. They help plan for the future. They listen.
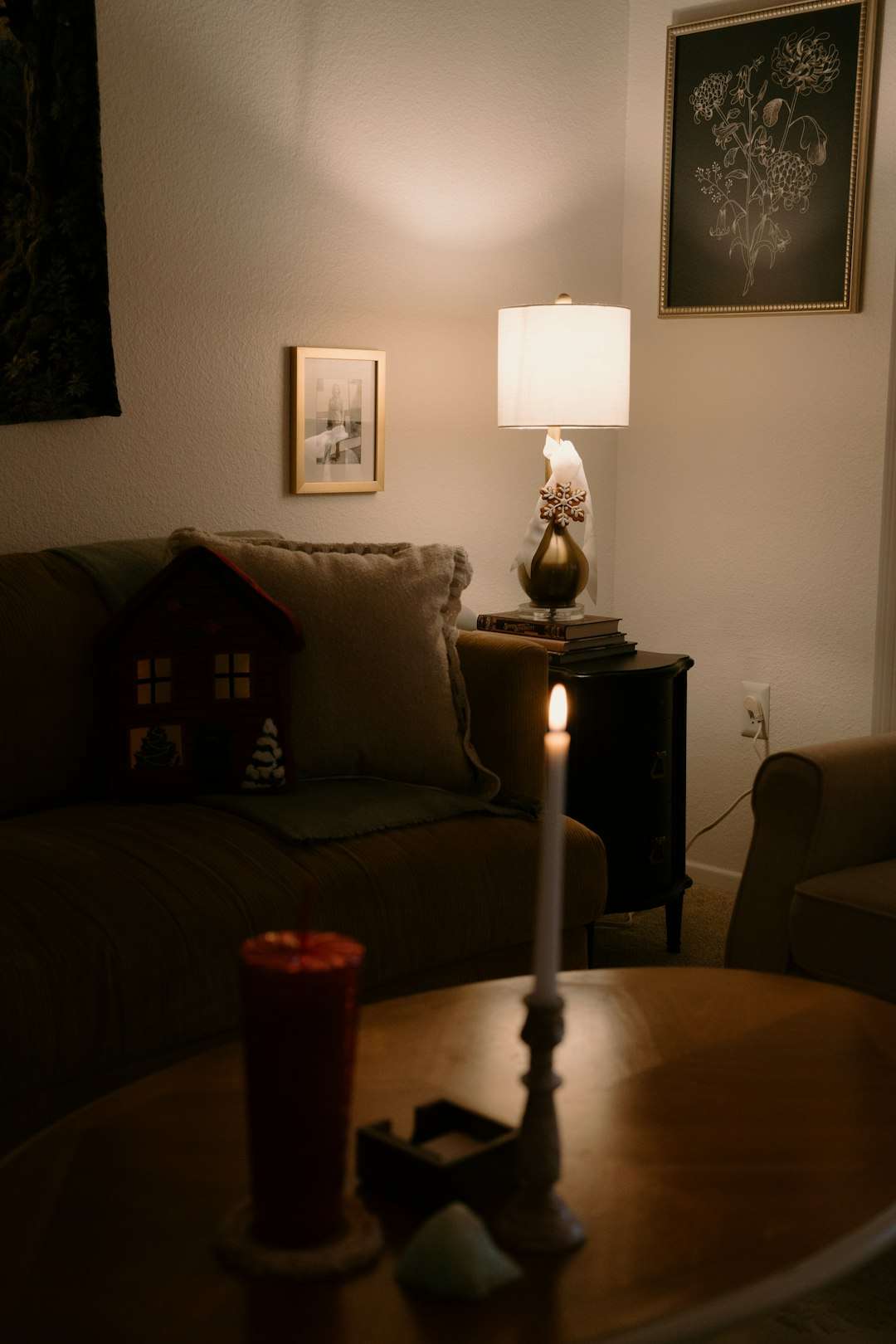
Why Home Makes a Difference
Hospitals can feel busy. Loud. Bright. Machines beep. Staff change shifts. It can be stressful. At home, life feels slower. More personal.
Being at home allows people to:
- Sleep in their own bed
- Eat favorite foods
- Be close to pets
- Set their own schedule
- Have family around anytime
These small comforts can lift the spirit. And when the spirit feels better, the body often feels better too.
Quality of life is not just about medical charts. It is about moments. Watching a grandchild play. Sitting in the garden. Listening to music. These little things matter.
Pain Management Made Simple
Pain is one of the biggest fears people have. The good news is this: pain can almost always be managed.
Palliative care teams use many tools:
- Medications
- Nerve blocks
- Physical therapy
- Relaxation techniques
- Massage
- Heat or cold therapy
The key is balance. The team adjusts treatment as needed. They listen carefully. If something is not working, they change it.
No one should suffer in silence. Speaking up about pain is important. It helps the team help you.
Emotional Support for Everyone
Serious illness affects more than the body. It touches emotions. It touches relationships. Patients may feel fear. Anger. Sadness. Even guilt.
Families feel stress too. They worry. They get tired. They may feel overwhelmed.
Palliative care supports everyone involved. Social workers and counselors offer space to talk. Support groups connect families with others in similar situations. Even simple check-ins can ease heavy hearts.
Caregivers need care too. Breaks are important. Rest is not selfish. It is necessary.
Spiritual and Personal Meaning
Serious illness often brings big questions. What matters most? What legacy will I leave? What gives my life meaning?
Palliative care teams respect all beliefs. Religious. Spiritual. Or none at all. Chaplains or spiritual counselors can visit. Or simply listen.
Sometimes, comfort comes from:
- Prayer or meditation
- Life review conversations
- Music
- Writing letters
- Creating memory books
These moments can bring peace. They can also bring families closer together.

Better Communication, Less Confusion
Medical information can be confusing. Big words. Fast explanations. Many choices.
Palliative care teams help translate. They explain options in simple terms. They help patients clarify goals.
Some helpful questions include:
- What do I hope for most?
- What worries me the most?
- What trade-offs am I willing to make?
- Where do I want to receive care?
When goals are clear, decisions feel less scary. Everyone understands the plan. That reduces stress.
Daily Life Gets Easier
Palliative care at home also helps with practical needs. That can include:
- Coordinating medications
- Arranging medical equipment
- Scheduling visits
- Teaching family members how to provide care
Equipment might include hospital beds, oxygen machines, or shower chairs. The team shows caregivers how to use them safely.
Knowledge builds confidence. Confidence reduces anxiety.
Image not found in postmetaPalliative Care vs Hospice Care
People often mix these up. Here is a simple comparison:
| Feature | Palliative Care | Hospice Care |
|---|---|---|
| When it begins | At any stage of serious illness | Usually when life expectancy is 6 months or less |
| Curative treatment allowed? | Yes | No, focus is comfort only |
| Location | Home, hospital, clinic | Home, hospice center, nursing facility |
| Main goal | Improve quality of life | Comfort at end of life |
Both focus on comfort. Both support families. The timing is the main difference.
The Power of Small Joys
When someone is very sick, joy may look different. It might be small. But it is still powerful.
Examples of simple joys at home:
- Sunlight through a window
- A favorite movie
- Homemade soup
- A visit from a friend
- A pet curled up on the bed
Palliative care teams often encourage families to focus on these moments. They ask, “What makes a good day for you?” The answer guides the care plan.
Good days are still possible. Even in serious illness.
Support for Caregivers
Caring for a loved one at home is meaningful. It is also hard work. Caregivers may lift, bathe, feed, and manage medicines. They may wake up at night. They may juggle jobs and children too.
Palliative care offers:
- Training in caregiving skills
- Respite care options
- Emotional counseling
- Help with community resources
Caregivers should watch for signs of burnout. These include:
- Constant fatigue
- Irritability
- Sleep problems
- Loss of appetite
- Feeling hopeless
Asking for help is not weakness. It is wisdom.
Planning Ahead Brings Peace
Talking about future wishes can feel uncomfortable. But it brings relief. Advance care planning includes:
- Living wills
- Healthcare proxies
- Do Not Resuscitate orders
- Documenting personal wishes
When plans are written down, families do not have to guess. They can feel confident they are honoring their loved one’s wishes.
That peace of mind is priceless.
How to Get Started
If you think palliative care at home might help, start by asking a doctor. Many hospitals have referral programs. Insurance, including Medicare and Medicaid, often covers it. Private insurance usually does too.
Ask questions like:
- What services are included?
- How often will the team visit?
- Who do we call after hours?
- What costs should we expect?
Clear information helps families prepare.
Living Fully, Even Now
Palliative care at home changes the focus. It shifts from “How do we cure this?” to “How do we live well now?”
That shift can be powerful. It brings control back to the patient. It centers care around personal values. It honors dignity.
Serious illness is hard. There is no denying that. But comfort is possible. Laughter is possible. Connection is possible.
Improving quality of life through palliative care at home is about wrapping medical support around real life. It is about easing pain. Calming fears. Creating meaningful moments. All in the place that feels most like you.
And sometimes, the best medicine is simply being home.